A Healthy Smile for Two
Maintaining good oral health during pregnancy is more than a cosmetic concern; it directly influences maternal and fetal well‑being. Hormonal shifts increase the risk of gingivitis and periodontal disease, and untreated gum inflammation has been linked to higher rates of preterm birth, low birth weight, pre‑eclampsia, and gestational diabetes. Cavities also rise because of altered eating patterns and morning‑sickness‑related acid exposure, and one in four women of child‑bearing age have untreated decay that can be passed to their child. Bacterial species such as Streptococcus mutans are transferred through saliva sharing, spoon‑feeding, and kissing, raising the infant’s chance of early childhood caries, which in turn can cause pain, missed school days, and costly dental treatment. Prenatal dental counseling—delivered through initiatives like the CDC’s Protect Tiny Teeth program—provides infographics, videos, and talking points that empower expectant mothers to brush twice daily with fluoride toothpaste, floss, limit sugary snacks, and schedule regular cleanings. Referral to a dentist, especially in the second trimester, ensures safe treatment of gum disease and cavities, protecting both mother and baby and establishing a foundation for the newborn.
Oral Health Matters for Mom and Baby
 | |
| Hormonal Changes and Gingivitis Risk | |
| During pregnancy, Estrogen rises ten‑fold and progesterone thirty‑fold during pregnancy (up to ten‑fold and thirty‑fold, respectively). These hormonal shifts increase blood flow to the gums, making them more red, swollen, and prone to inflammation. As a result, 60‑75 % of pregnant women develop gingivitis, an early stage of periodontal disease. Maintaining diligent oral hygiene—brushing twice daily with fluoride toothpaste and flossing daily—helps control plaque and reduces gum swelling. |
Untreated Gum Disease and Preterm Birth
If untreated gingivitis can progress to periodontitis, it may lead to adverse outcomes. Periodontitis is linked to preterm birth and low birth weight. Prompt professional cleanings and, when needed, scaling and root planing in the second trimester can interrupt this cascade, protecting both mother and baby.
Bacterial Transmission and Early Childhood Caries
Mothers with untreated cavities or gum disease harbor high levels of cariogenic bacteria such as Streptococcus mutans. These bacteria are easily transferred to infants through saliva sharing (e.g., sharing spoons or cleaning a pacifier with a mouth). Children of mothers with high levels of untreated cavities are more than three times as likely to develop cavities themselves. Early oral‑health counseling, preventive dental visits during pregnancy, and education on infant oral hygiene are essential steps to break this cycle and give the child a healthier start.
Safe Dental Care Throughout the Trimesters
 | ||
| What is the recommended dental management plan for a pregnant patient? | ||
| Pregnant patients should receive routine preventive care—cleanings, examinations, and oral‑hygiene counseling—each trimester. Cleanings and exams are safe at any stage; radiographs are performed only when essential and always with lead shielding. Elective procedures are postponed until the second trimester or after delivery, while urgent treatments (e.g., treatment of acute infection, pain relief, extractions) are safely carried out in the second trimester. The dentist emphasizes strict plaque control, a calcium‑ and vitamin‑D‑rich diet, and twice‑daily fluoride brushing, coordinating with the obstetrician as needed. |
Is dental work safe during the first trimester? Yes. Preventive cleanings, examinations, and urgent care (e.g., treatment of a painful cavity) are safe in the first trimester. Diagnostic X‑rays with proper lead shielding cause negligible fetal exposure. Elective cosmetic work (teeth whitening, veneers) should be delayed. Patients must inform the dentist of their pregnancy so minimal effective doses of lidocaine and pregnancy‑safe antibiotics (penicillin, amoxicillin, clindamycin) are used.
When is the safest period for dental treatment during pregnancy? The second trimester (≈weeks 14‑27) is the optimal window for non‑urgent procedures such as fillings, crowns, or minor oral surgery. Mother is more comfortable supine, and organogenesis is complete, reducing theoretical risks. Preventive cleanings are safe in any trimester; emergencies are treated promptly at any stage.
Which dental procedures should be avoided while pregnant? Elective cosmetic procedures (whitening, bonding, veneers) and non‑essential oral surgeries should be postponed until after delivery. Routine diagnostic X‑rays can be delayed, especially in the first and third trimesters. Prolonged chair time in the third trimester should be minimized to avoid supine hypotension.
What are the dangers of dental work in the third trimester? Extended supine positioning can cause supine hypotension, reducing uterine blood flow. Stress and discomfort may increase the risk of pre‑term labor. Therefore, elective work is deferred; only urgent care is performed, using minimal anesthesia and proper shielding for any needed radiographs.
What guidelines does ACOG provide for dental care in pregnancy? ACOG states that preventive, diagnostic, and restorative dental care—including radiographs with shielding and lidocaine with or without epinephrine—are safe at any stage. Urgent procedures should not be delayed. Obstetricians and dentists should coordinate care, and topical fluoride varnish is preferred for pregnancy‑related enamel protection.
Gum Disease, Cavities, and Tooth Loss
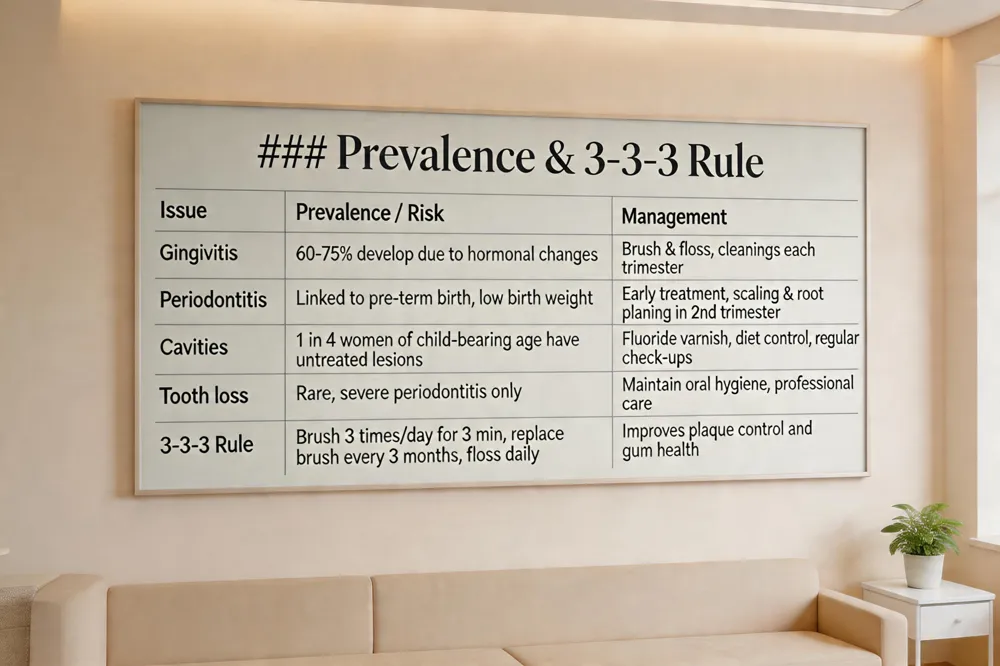 | ||
| Pregnant women experience a dramatic rise in gum inflammation: 60 %–75 % develop gingivitis due to heightened estrogen and progesterone, which increase blood flow and plaque‑related swelling. If gingivitis is left untreated, it can progress to periodontitis, a deeper infection linked to low‑birth‑weight and preterm delivery. While cavities are also more common—one in four women of child‑bearing age have untreated lesions—most are manageable with preventive care. Untreated decay can be transmitted to infants via saliva, making children of mothers with high cavity loads three times more likely to develop early childhood caries. |
How common is it to lose teeth during pregnancy? Tooth loss is rare. The majority of pregnant patients only experience temporary gum inflammation. Only a small fraction progress from gingivitis to severe periodontitis that threatens tooth stability. Prompt brushing, flossing, and regular dental cleanings dramatically lower the risk; thus, losing a tooth while pregnant is the exception rather than the rule.
What is the 3‑3‑3 rule for teeth? This simple daily guideline advises brushing three times a day—typically after meals—for three minutes each session, using a soft‑bristled brush with fluoride toothpaste and avoiding immediate rinsing to let fluoride act. Replace the brush or electric head every three months. Pair this with daily flossing or interdental cleaning for optimal plaque control.
Maintaining these habits, together with routine dental visits (ideally in the second trimester), helps prevent gingivitis, cavities, and the unlikely event of tooth loss, protecting both mother and child.
Medications, Anesthetics, and Radiographs
 | ||
| Dental care is safe at any stage of pregnancy when evidence‑based precautions are followed. Lidocaine—an FDA Category B local anesthetic—is the preferred agent for pregnant patients; it may be used with a low‑dose vasoconstrictor (≤0.05 mg epinephrine per cartridge) to control bleeding and prolong anesthesia without harming the fetus. Epinephrine‑containing formulations are considered safe when the minimal effective amount is administered, and higher concentrations should be avoided. |
For infections, the safest antibiotics are those also Category B, such as penicillin, amoxicillin, and clindamycin; they effectively treat oral infections without fetal risk. Tetracycline and fluoroquinolones are contraindicated.
Radiographic imaging is also permissible. Modern digital X‑rays emit negligible radiation (<0.01 mrad); when a lead apron (and thyroid collar when indicated) is used, fetal exposure remains far below the threshold for harm. Routine diagnostic X‑rays should be performed only when clinically necessary, and the second trimester is the optimal window for elective imaging.
Answers to key questions
- Is epinephrine safe in dental anesthesia for pregnant patients? Yes—low‑dose epinephrine (≤0.05 mg per cartridge) is safe and helps control bleeding without adverse fetal effects.
- Which local anesthetics are preferred during pregnancy? Lidocaine, preferably with low‑dose epinephrine or without a vasoconstrictor, is the anesthetic of choice; other Category B agents (e.g., mepivacaine) may be used as needed.
- What does the ADA say about dental care during pregnancy? The ADA recommends continued preventive care, including cleanings, exams, and shielded X‑rays, throughout pregnancy; necessary diagnostic and restorative treatments are safe, especially in the second trimester, and untreated oral disease should not be delayed.
Nutrition, Home Care, and Daily Practices
 | |
| Good oral hygiene during pregnancy starts with brushing twice daily using a soft‑bristled toothbrush and fluoride toothpaste and daily flossing to disrupt plaque and remove food debris. Fluoride varnish applied by a dentist offers extra protection for vulnerable enamel. Nutrition plays an equally vital role: calcium‑rich foods such as low‑fat dairy, leafy greens and fortified plant milks, combined with adequate vitamin D—via sunlight exposure, fortified foods, or supplements—support tooth mineralization and overall bone health for mother and baby. Pregnant women should limit sugary snacks and acidic drinks, choosing water (ide fluoridated) and balanced meals to keep oral pH stable. Morning‑sickness can expose teeth to stomach acid; the safest approach is to rinse the mouth with plain water or a diluted baking‑soda solution (1 tsp baking soda in 1 cup water) after vomiting, then wait at least 30 minutes before brushing to avoid enamel erosion. |
How does a mother’s oral health affect her baby? Untreated gum disease and cavities can increase systemic inflammation and allow bacteria to reach the placenta, raising the risk of pre‑term birth and low birth weight. Harmful bacteria can also be transmitted to the infant after birth, elevating the child’s likelihood of early childhood caries. Maintaining a healthy mouth through regular dental visits, proper hygiene, and a nutritious diet protects both mother and baby.
How can a pregnant woman protect her teeth? Brush twice a day with fluoride toothpaste, floss daily, and use a soft brush. Limit sugary foods, stay hydrated, and consume calcium‑rich foods and vitamin D. Morning rinse with baking soda before brushing, and inform the dentist of pregnancy status for safe X‑rays and treatments.
Access, Insurance, and Community Resources
 | |
| Dental coverage for pregnant women in the United States typically includes preventive services—routine exams, cleanings and periodontal care—along with diagnostic X‑rays and necessary restorative work such as fillings, crowns, or extractions when medically indicated. Many private plans (e.g., Delta Dental PPO and Premier) add an extra exam and cleaning specifically for pregnancy. Medicaid’s dental benefit varies by state; in Texas it is limited, so pregnant patients should verify eligibility and benefits, and SH coaches can offer the caregivers protection oral‑health services of the “Protect Tiny Teeth” initiative provides multilingual infographics, videos, and talking points to help providers educate expectant mothers and connect them with low‑cost or free care. Texas women can also access free or low‑cost dental services through the state‑run “Smiles for Moms and Babies” program, which links patients to community health clinics and university dental schools, and through Medicaid‑eligible plans such as STAR, CHIP, or STAR Kids that cover preventive and comprehensive dental care without out‑of‑pocket costs. ACOG guidelines emphasize that preventive, diagnostic, and restorative dental care—including radiographs with proper shielding and local anesthesia with epinephrine—is safe at any trimester; urgent procedures should not be delayed, and obstetricians and dentists should coordinate care, especially for high‑risk pregnancies. Topical fluoride varnish is preferred when needed to minimize nausea. |
V Dental’s Pregnancy‑Friendly Services
 | |
| V Dental in Live Oak, Texas, integrates evidence‑based oral‑health care into prenatal health. The practice offers comprehensive preventive services—routine cleanings, fluoride‑varnish applications, and personalized oral‑hygiene counseling that emphasize twice‑daily brushing with fluoride toothpaste, daily flossing, and diet tips to limit sugary snacks and neutralize acid after morning‑sickness (CDC ‑ Protect Tiny Teeth; ACOG; HRSA). Expectant mothers receive safe imaging: modern digital X‑rays, intraoral cameras, and low‑dose CBCT 3‑D scans that provide precise diagnostics while delivering radiation doses far below fetal‑harm thresholds when lead shielding is used (ADA; CDC; ACOG). V Dental’s flexible financing options and individualized treatment plans remove financial barriers, allowing women of all income levels to access needed preventive and restorative care during pregnancy. Scheduling is tailored for pregnant patients—appointments can be set at convenient times, with chair positioning (slight left‑tilt or pillow support) to maintain uterine blood flow and comfort during the second trimester, the optimal window for most dental work. By aligning with CDC’s Protect Tiny Teeth toolkit and ACOG recommendations, V Dental ensures that both mother and baby receive the oral‑health protection essential for a healthy pregnancy and a strong start to the child’s lifelong dental health. |
Take the First Step Toward a Healthy Pregnancy Smile
Begin your prenatal oral‑health plan by scheduling a dental exam early in pregnancy—ideally in the first trimester—so the dentist can assess gum health, detect early cavities, and provide a baseline for future care. The CDC’s Protect Tiny Teeth initiative and the ADA both stress that preventive cleanings and exams are safe at any stage and can help reduce the risk of gingivitis, which affects 60‑75 % of expectant mothers and is linked to preterm birth and low birth weight.
Adopt the simple “3‑3‑3” routine: brush twice daily (morning and night) for at least three minutes with fluoride toothpaste, floss for three minutes once a day, and limit sugary snacks to three servings per day. This regimen combats the hormonal surge that swells gums and the extra snacking that raises cavity risk. If vomiting occurs, rinse with a teaspoon of baking soda in a cup of water to neutralize acid before brushing.
V Dental in Live Oak, Texas, supports this plan with modern tools—digital X‑rays, intra‑oral cameras, and CBCT 3‑D imaging—that deliver low‑dose, precise diagnostics while protecting the fetus. The practice also offers flexible financing and personalized treatment plans, making it easy for pregnant patients to receive timely cleanings, fluoride varnish, and any necessary restorative work without financial delay.
